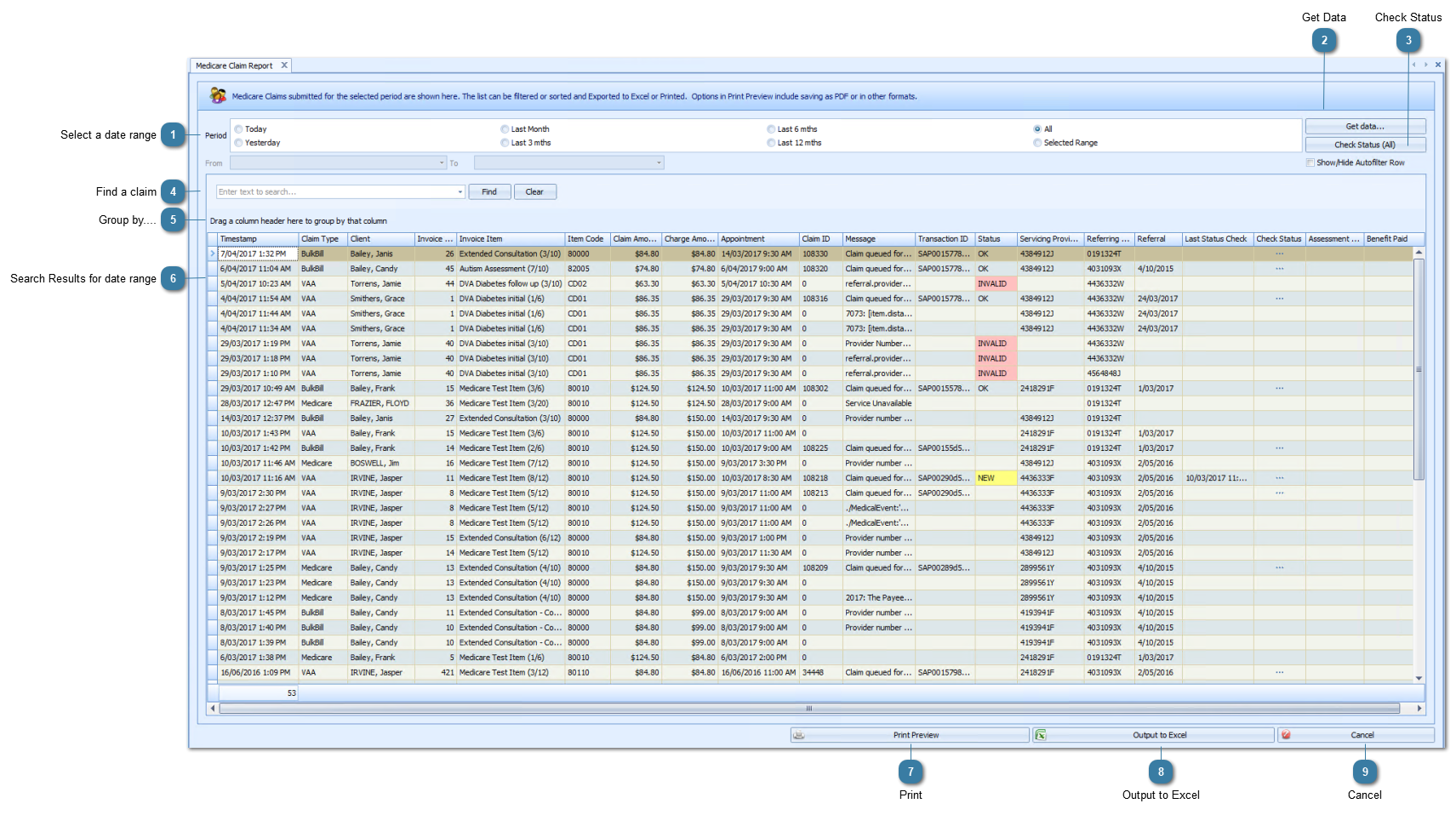
Search Results for date rangeSearch results for the above date range.
Fields available:
Timestamp - date and time the claim was sent
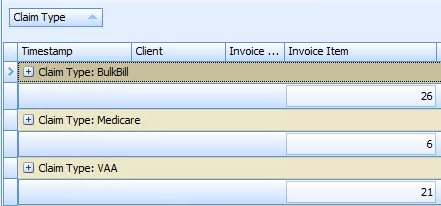
Claim Type - whether its Bulk Bill, VAA (DVA), Medicare (Patient Claim)
Client - who the claim is for
Invoice No. - Invoice claimed
Invoice Item - Item description
Item Code - Medicare or DVA Item Code
Claim Amount - Amount claimed
Charge Amount - Amount charged. For DVA and BB this must be the same as Claim Amount.
Appointment - Appointment Date and Time
Claim ID - Claim ID assigned by Bp Allied
Message - any error messages relating to the claim will be stored here. If it has been successfully sent then the message is "Claim queued for sending"
Transaction ID - ID assigned by Claiming.com.au
Servicing Provider ID - The provider number of the medical practitioner rendering the service(s) as allocated by Medicare
Referring Provider ID - The referring provider number
Referral Date - The date the referral was issued
Last Status Check - date and time when the status was last checked
Check Status - Click to check the status if an individual claim.
Assessment Note - Includes any rejection codes that come back from Medicare if the claim could not be successfully processed.
Benefit Paid - amount paid by Medicare or DVA. This could include Loading and KM payments
|